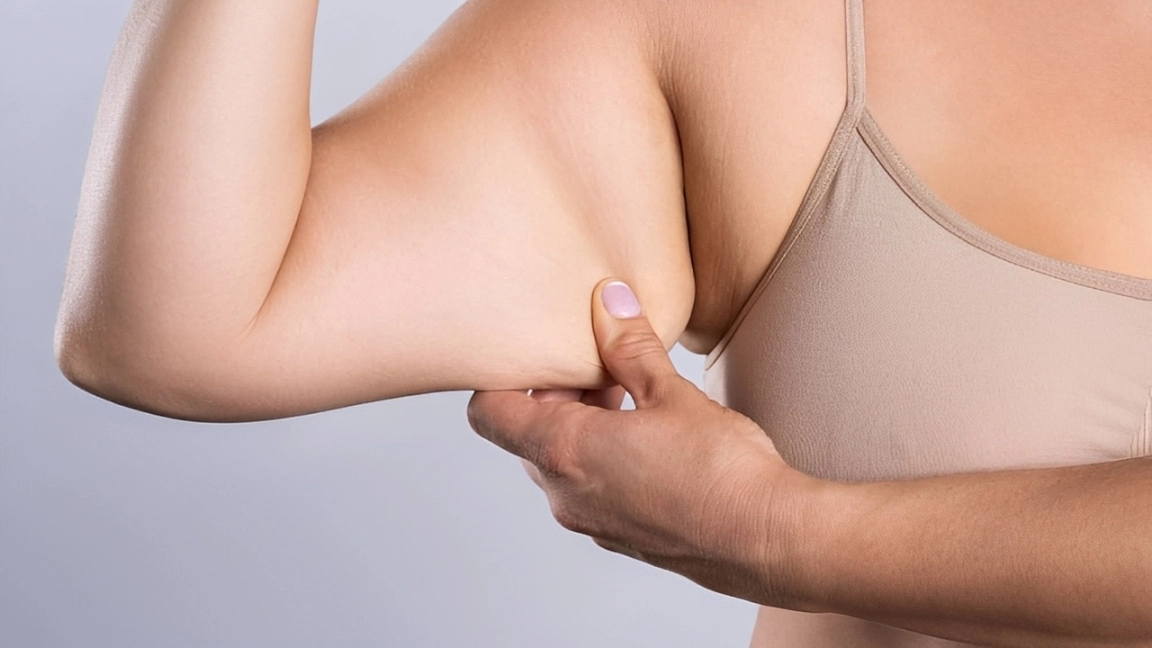
The frustration of having thick arms that are disproportionate, despite maintaining a strict diet and engaging in exercise, is a painful reality for thousands of women. For too long, this accumulation of fat has been misconstrued as overweight or a supposed lack of discipline, leaving patients trapped in a cycle of misdiagnosis and without a real solution.
At Lipedema Advanced Care, we understand your story. Lipedema is a chronic, progressive disease of the adipose tissue, with hormonal and genetic origins, that affects the extremities and, in more advanced stages, the arms. It is not your fault; lipedema fat does not respond to diet or exercise. Here, we offer you a precise diagnosis and the most effective treatment to regain lightness and quality of life.
What is Lipedema in the Arms?
Lipedema is a chronic and progressive disorder of fat tissue distribution that predominantly affects women, with estimates suggesting that between 6% and 15% of the global female population suffer from it.
When the disease manifests in the upper limbs, it presents as an abnormal, pathological, and typically symmetrical accumulation of fat tissue, mainly in the upper part of the arms. This accumulation can even extend to the forearms. A defining characteristic is that this fat stops abruptly: the wrists and hands are generally unaffected.
Lipedema in the arms is not a simple aesthetic problem; it is a medical condition that causes pain, limits mobility, and generates a significant emotional impact.
Why Are My Arms Thick? Causes of Lipedema in the Arms
The exact cause of lipedema is not fully understood, but there is a strong consensus that its origin is multifactorial, driven by a combination of genetic predisposition and hormonal factors.
Genetic Factors
Lipedema is strongly believed to have a clear genetic component. It is estimated that approximately 50% of women who suffer from lipedema have a family history of the disease.
Influence of Hormonal Changes
Hormonal changes play a crucial role as triggers or aggravators of the condition. This explains why the disease predominantly affects women.
The disease usually appears or worsens during periods of significant hormonal fluctuations in a woman’s life:
Puberty.
Pregnancy.
Menopause.
Symptoms of Lipedema in the Arms
Lipedema in the arms is distinguished from common fat by a set of sensory and physical symptoms that define its pathological nature.
Disproportionate Fat Accumulation in the Arms
This is one of the most noticeable symptoms of lipedema. The fat accumulation is symmetrical and disproportionate relative to the torso. This pathological fat distribution makes the affected arms appear heavy or swollen, often described as having a “column-like” appearance or looking like “tree trunks”. Disproportion can occur even in women with normal or low body weight.
Pain and Sensitivity to Touch
Lipedema is a painful medical condition, and chronic pain is a characteristic symptom.
Sensitivity to touch: The arms are hypersensitive and painful. Pressure, a hug, or even the friction of clothing or a caress can cause sharp, inexplicable pain.
Pain at rest: The pain can be constant or intermittent and is experienced even at rest.
Easy Bruising in the Arms
The tendency for bruises (hematomas) to appear easily is a key feature of lipedema. Bruises appear very easily, sometimes from minimal bumps or even with no obvious cause. This is due to the capillary fragility in the affected tissue.
Persistent Swelling in the Arms
The pathological fat accumulation causes noticeable and persistent swelling in the arms, which contributes to a constant feeling of heaviness and fatigue. Unlike common swelling from fluid retention, lipedema swelling does not significantly improve with limb elevation.
Changes in Skin Texture and Formation of Adipose Nodules
The accumulated fat can feel harder than normal abdominal fat, and sometimes presents nodularity. These adipose nodules or lumps can be felt under the skin when palpated, and they are frequently tender to the touch. Over time, the skin may thicken or develop an irregular, dimpled appearance, similar to cellulite.
Diagnosis of Lipedema in the Arms
Lipedema remains an underdiagnosed disease. It is common for the diagnosis to be delayed between 5 and 7 years, a long journey that severely impacts patients’ quality of life. The main difficulty lies in its confusion with other conditions.
Clinical Evaluation by a Specialist
The diagnosis of lipedema is primarily clinical and must be performed by a specialist.
Differential Diagnosis: It is crucial to differentiate lipedema from obesity (which responds to diet and exercise), cellulite (which is generally not painful or does not cause bruises), and lymphedema.
Physical Inspection: The specialist evaluates body disproportion, resistance to weight loss in specific areas, pain upon touch, and the ease of bruising.
Complementary Imaging Tests
Although the diagnosis os lipedema is clinical, the specialist may use imaging tests to rule out other pathologies or assess the condition of the tissues.
Importance of Early Diagnosis
Early diagnosis is crucial to manage symptoms, establish an appropriate and personalized treatment plan, and prevent the progression of the disease to more advanced stages.
Specialized Surgery: The Most Effective Treatment to Eliminate Lipedema in the Arms
Lipedema is resistant to conventional weight loss methods. Therefore, when conservative measures are insufficient, surgical intervention is presented as the most effective strategy for eliminating the pathological fat tissue, alleviating chronic pain, and improving mobility.
Conservative Treatments
Conservative therapies are a fundamental pillar in symptom management and are integrated into all phases of treatment.
| Conservative Therapy | Key Goal for Arm Lipedema |
| Compression Therapy | Control swelling (edema), reduce pain/discomfort, and slow the disease’s progression. |
| Manual Lymphatic Drainage (MLD) | Stimulate lymphatic fluid circulation, helping to reduce swelling, pain, and feelings of heaviness. |
| Adapted Physical Exercise | Improve mobility, strengthen muscles, reduce heaviness, and activate the lymphatic system. |
| Anti-inflammatory Diet | Reduce systemic inflammation to improve pain and other symptoms. |
Compression Therapy
The use of custom-made compression garments (such as sleeves or arm bands) is fundamental to controlling swelling (edema), reducing pain and discomfort, and slowing the progression of the disease.
Manual Lymphatic Drainage
Manual Lymphatic Drainage (MLD) is a gentle massage technique performed by a specialized physiotherapist that stimulates the circulation of lymphatic fluid. This therapy is effective in reducing swelling, alleviating pain, and reducing feelings of heaviness.
Adapted Physical Exercise
Low-impact exercises, such as swimming, yoga, or walking, are recommended to improve mobility, reduce heaviness and fatigue, and activate the lymphatic system without aggravating the pain.
Anti-inflammatory Diet and Nutritional Supplements
An anti-inflammatory diet, rich in fruits, vegetables, lean proteins, and healthy fats, and low in processed foods and sugars, is crucial to reduce systemic inflammation and improve symptoms.
Complementary Therapies
For symptomatic pain management, specialists may resort to anti-inflammatory drugs and analgesics (such as NSAIDs). In cases of severe chronic pain, medications for neuropathic pain, such as gabapentin or pregabalin, may be considered.
Surgical Treatments
Lipedema liposuction techniques are specialized; unlike aesthetic liposuction, they aim to be less traumatic and preserve lymphatic structures.
Tumescent Liposuction: Involves injecting a solution that facilitates extraction and reduces blood loss and postoperative pain control.
Power-Assisted Liposuction (PAL): Uses a vibrating cannula for a more complete and precise fat removal, beneficial for large areas.
WAL Liposuction: The Most Advanced and Least Invasive Technique for Lipedema
Water-Assisted Liposuction (WAL or WALE) is one of the most advanced techniques and the procedure of choice at Lipedema Advanced Care for the treatment of lipedema in the arms.
Advantages of WAL Liposuction
WAL uses a gentle jet of water to break down and remove the pathological fat tissue. This mechanism offers key and substantial benefits:
| Key Advantage | Benefit for the Lipedema Patient |
| Minimum Trauma and Lymphatic Preservation | The technique causes less trauma to the surrounding tissues, which helps preserve the vascular and lymphatic structures. |
| Faster Recovery Times | Reduced tissue trauma results in faster recovery times than traditional techniques. |
| Fewer Bruises and Swelling | The gentleness of the method reduces the occurrence of bruises and postoperative inflammation. |
| High Contour Precision | Allows for more precise and controlled fat removal, leading to smoother and more uniform results in body contouring. |
Surgical Process and Essential Postoperative Care (Compression, MLD)
Meticulous postoperative care is essential to ensure optimal recovery and lasting results.
Essential compression garments: The use of compression garments is mandatory and essential during recovery to reduce swelling and promote smooth healing.
Early mobilization: Light walking immediately after surgery is recommended. This is crucial to promote circulation and prevent the formation of blood clots.
Postoperative lymphatic drainage: Manual Lymphatic Drainage (MLD) sessions are essential and frequently recommended to manage residual inflammation and accelerate the reduction of postoperative edema.
Recovery times: Most patients can resume non-strenuous work within 1-2 weeks. Full recovery, including the resumption of all physical activities, usually takes between 4 and 6 weeks.

Short- and Long-Term Results
Surgery is not a definitive cure, as lipedema is a chronic, progressive condition. However, it provides substantial and long-lasting functional results:
Significant symptom improvements: Substantial postoperative improvements have been demonstrated in spontaneous pain, edema, ease of bruising, and mobility. The patient usually notices a great improvement in symptoms immediately after the operation.
Proven durability: Long-term follow-up studies have shown that the positive effects of liposuction can last up to 12 years after the operation without significant worsening of symptoms.
Brachioplasty (optional): In advanced cases where fat removal leaves residual excess skin, an Arm Lift (Brachioplasty) may be performed in a second surgical step to correct the sagging skin and improve the contour. It is recommended to be done sequentially (first liposuction and then the lift).
The Holistic Approach and Comprehensive Management of Lipedema in the Long Term
Successful long-term management of lipedema requires a comprehensive and continuous treatment approach. The holistic approach of Lipedema Advanced Care addresses the person in their entirety, not just the physical aspects of lipedema, but also their emotional and mental well-being.
Development of a Personalized Treatment Plan
Our multidisciplinary team, which includes specialized plastic surgeons, nutrition specialists, and physiotherapists, works together to design a personalized treatment plan. This plan integrates preoperative conservative therapies, specialized surgical intervention, and meticulous postoperative care
Emotional and Psychological Support
Lipedema carries a deep physical and emotional burden. We offer constant support to manage the psychological impact of living with a chronic disease.
We foster a supportive environment where patients can connect with other women going through similar situations.
Continuous Monitoring of Treatment
Long-term management is essential to minimize complications and prevent the condition from worsening. We encourage self-management and continuous monitoring to maintain surgical results and general health.
Prevention and Daily Care for Lipedema in the Arms
Once the pathological fat is removed, commitment to lifestyle is fundamental for long-term success.
Stratagies to Minimize Symptoms
Strategies focus on controlling inflammation and pain:
Continue with an anti-inflammatory diet to reduce systemic inflammation.
Use analgesics or anti-inflammatories, if necessary, to manage residual chronic pain.
Maintain continuous manual lymphatic drainage, as indicated by the physiotherapist.
Importance of a Healthy Lifestyle
Maintaining a healthy lifestyle, including adapted physical exercise and a balanced diet, is necessary to maintain surgical results and improve general well-being, as it helps to prevent the disease’s progression.
Appropriate Use of Compression Garments
The continuous use of graded compression garments is fundamental in the chronic management of lipedema to reduce swelling and discomfort in the arms. The type and intensity of compression (Ccl 1 to Ccl 4) must be determined by your medical specialist.
| Comparison Criterion | Lipedema in the Arms (Disease) | Common Obesity (Generalized Accumulation) | Cellulite (Superficial) | |
| Fat Distribution | Symmetrical and disproportionate accumulation in limbs (arms/legs). Does not affect hands or feet. | Fat accumulation more generalized throughout the body, tending to be proportional. | Localized accumulation forming dimples (“orange peel”), mainly in hips, thighs, and buttocks. | |
| Response to Diet/Exercise | Resistant fat: Pathological fat is not eliminated with caloric restriction or physical exercise. | Responds to diet and exercise. | Can improve with diet and exercise. |
|
| Pain and Sensitivity | Frequently painful and sensitive to touch or pressure. | Generally not painful. | Not usually painful. |
|
| Bruising | Tendency to bruise easily. | Not a characteristic symptom. | Does not cause bruising. |
|
Take the first step toward your well-being. We invite you to schedule a consultation with our team at Lipedema Advanced Care to receive an expert and comprehensive evaluation in Valencia.

Dr Alexo Carballeira trained at prestigious national and international universities, perfecting his technique alongside world leaders in plastic surgery such as Dr Ivo Pitanguy and Dr Pedro Cavadas. He holds a degree in Medicine and is a specialist in Plastic, Aesthetic and Reconstructive Surgery. He also has an International Master's Degree in Reconstructive Microsurgery.